Be honest: have you ever finished peeing, zipped up, and then… surprise! There’s still a leak? Or felt that sudden gotta‑go‑right‑now urgency, struggled to get your stream started like an old car on a cold morning, or found yourself waking up at night because your bladder apparently set its own alarm?
If any of that sounds familiar, you’re not alone. In fact, nearly half of Canadian men over 40 experience urinary or sexual changes, and many notice symptoms years before they ever receive a diagnosis. And no, this isn’t just “getting old.” These are some of the most common early signs that your prostate (and pelvic floor) may be under strain.
This guide explains why prostate health matters for every man over 40, what symptoms to watch for, and how evidence‑based strategies can protect your urinary function, sexual health, and long‑term quality of life.
Why the Prostate Matters More Than You Think
The prostate may be small, but its influence is huge. Sitting just below the bladder and wrapped around the urethra, it plays a central role in:
- Urination: Stream strength, frequency, and how well the bladder empties
- Sexual function: Ejaculation volume, orgasm intensity, and erection quality
- Pelvic nerve signaling: Discomfort is often felt far away from the gland itself
This matters because prostate-related conditions are incredibly common in Canada. By age 60, over 40–50% of Canadian men will have some degree of prostate enlargement (BPH), often with symptoms that quietly creep in long before anything shows up on lab work.
Even mild enlargement, inflammation, or pelvic floor tension can ripple across multiple systems, often before blood work or imaging flags a problem.
Early Warning Signs You Shouldn’t Ignore
These symptoms are common, but they’re not “normal aging,” and they’re not something you just have to live with:
- Post‑void dribbling or leakage
- Sudden urgency or feeling like your bladder never fully empties
- Weak stream or difficulty starting urination
- Frequent nighttime bathroom trips
- Erectile instability or muted ejaculation
- Deep pelvic, rectal, perineal, or penile tip pressure
Think of these signs as early warning lights, not minor inconveniences.
What’s Really Going On? Cause and Effect Explained
Prostate symptoms rarely come from just one issue. They’re usually the result of several overlapping factors working together.
Hormonal Shifts and Aging
As men age, testosterone levels slowly decline, while dihydrotestosterone (DHT) remains active within prostate tissue. This combination can drive gradual prostate enlargement, known as benign prostatic hyperplasia (BPH), which affects nearly half of Canadian men by their 60s. The result can be urethral compression, a weaker urinary stream, difficulty emptying the bladder, and sometimes erectile dysfunction.
Chronic Inflammation
Chronic inflammation plays a major role. Metabolic dysfunction, visceral belly fat, gut inflammation, chronic stress, poor sleep, and environmental toxins can all irritate prostate tissue. Over time, this contributes to urgency, frequent urination, pelvic pressure, and changes in ejaculation – sometimes painful, sometimes muted.
Pelvic Floor Dysfunction
Another often‑missed contributor is pelvic floor dysfunction. The pelvic floor muscles can become too tight, too weak, or poorly coordinated. This can cause urinary retention or leakage, erectile instability, and deep discomfort felt in the pelvis, perineum, rectum, or even the tip of the penis. An estimated 9% of men experience chronic pelvic pain or prostatitis each year, many of whom are misdiagnosed or told nothing is wrong.
Naturopathic Insight: Prostate symptoms are rarely random. They’re predictable signals that something upstream needs attention. When we understand why symptoms are happening, we can target root causes instead of simply suppressing symptoms.
Lifestyle and Environmental Stressors
Lifestyle and environmental factors can quietly worsen prostate symptoms by disrupting hormones and increasing inflammation.
Excess body fat raises estrogen levels in men, contributing to hormonal imbalance, prostate growth, and inflammation. Poor sleep further lowers testosterone, affecting urinary control, erectile function, and pelvic muscle tone. Exposure to endocrine-disrupting chemicals (from plastics, pesticides, and personal care products) can interfere with hormone signaling, contributing over time to prostate enlargement, penile tissue changes, and worsening urinary and sexual symptoms.
Infection and Prostatitis
PSA Testing: What It Tells You (and What It Doesn’t)

Prostate‑Specific Antigen (PSA) is a protein marker of prostate activity, not a cancer test.
In Canada, PSA screening is typically offered between ages 50–70, but earlier testing is appropriate if symptoms are present or if there’s a family history or higher risk. This is important, given that 1 in 8 Canadian men will be diagnosed with prostate cancer, and early detection is a major reason survival rates remain high.
PSA can rise due to BPH, inflammation, urinary retention, recent ejaculation, or cancer.
General lab ranges (age‑dependent):
- <4 ng/mL: generally normal
- 4–10 ng/mL: elevated
- 10 ng/mL: higher suspicion
PSA ratio (free‑to‑total):
- <10–15%: higher malignancy risk
- 20–25%: more likely benign
PSA is a guide, not a diagnosis. Trends over time and clinical context matter most.
Prostate and Pelvic Floor Exams: Why They Matter
A digital rectal exam (DRE) assesses prostate size, texture, symmetry, nodules, and tenderness. It can also reproduce referred pelvic or rectal pressure.
A pelvic floor assessment evaluates:
- Muscle tone: hypertonic (tight) vs. hypotonic (weak)
- Coordination: contraction/release, and relaxation during urination
- Trigger points or nerve irritation
- Functional outcomes: like bladder emptying, erection, ejaculation, and pain
Given how common pelvic pain, erectile dysfunction, and urinary leakage are in Canadian men, these exams are often the missing piece. Many so‑called “prostate problems” are actually pelvic floor issues in disguise.
A Sample Daily Wellness Schedule for Prostate Health
Disclaimer: Consult your healthcare provider before starting any new exercise, diet, or supplement routine.
A consistent daily rhythm supports prostate and pelvic health, especially for men noticing early symptoms.
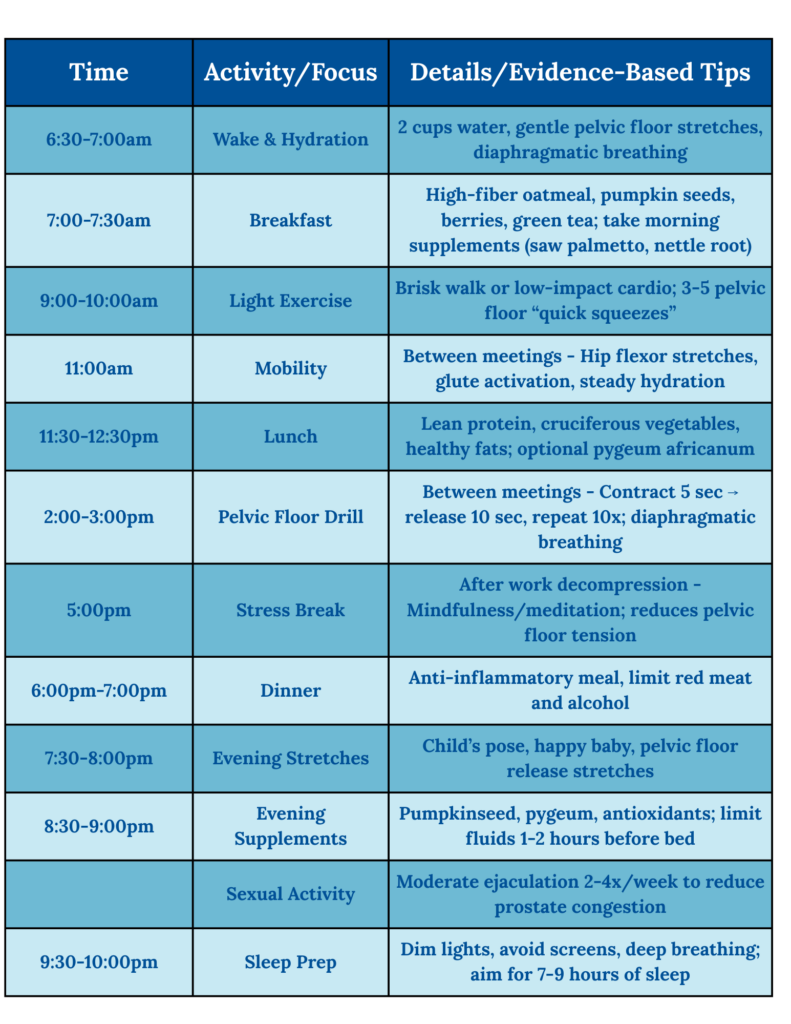
Evidence‑Based Management Options
1. Lifestyle Interventions (The Foundation of Care)
Lifestyle changes matter because they directly influence the most common prostate drivers affecting men:
- Weight management reduces estrogen dominance and DHT conversion
- Regular movement improves circulation, reduces inflammation, and supports erectile function
- Quality sleep supports testosterone production in deep sleep
- Stress management reduces pelvic floor tension and inflammatory signalling
- An anti‑inflammatory diet supports prostate health.
- Aim to reduce processed foods, added sugars, and alcohol
- Aim to increase vegetables, healthy fats, and other anti-inflammatory foods
2. Herbal and Nutraceutical Support

- Saw palmetto: may reduce DHT signalling and mild urinary symptoms
- Pygeum africanum: supports urinary flow and reduces nocturia and BPH-related irritation
- Nettle root: modulates androgen receptor activity and stromal tissue in the prostate
- Pumpkin seed extract: supports bladder function and reduces frequency
- Antioxidants: lycopene, green tea, and zinc offer additional support
These approaches tend to work best when started early, before symptoms become severe.
3. Pharmaceutical Options
- Alpha‑blockers (e.g. tamsulosin, alfuzosin): relax smooth muscle in the prostate and bladder neck, which improves urinary flow and reduces urgency
- 5‑alpha‑reductase inhibitors (e.g. finasteride, dutasteride): reduces DHT and prostate size over time and may prevent progression
- Anti‑inflammatories or antibiotics: for prostatitis or acute flare-ups (often misdiagnosed)
- Combination therapy: often used for moderate to severe symptoms with pelvic floor involvement
4. Pelvic Floor Therapy
Often overlooked, pelvic floor physiotherapy and biofeedback can dramatically improve pain, leakage, erections, and coordination, especially for men with chronic pelvic symptoms.
5. Ongoing Monitoring
- Annual PSA and symptom review
- Prostate and pelvic floor exams
- Hormone and inflammation lab monitoring when indicated
The best outcomes come from addressing hormonal, inflammatory, muscular, and functional factors together.
Final Thoughts
Prostate issues are common, predictable, and often manageable, but only if they’re addressed early. 1 in 8 men will face prostate cancer, over half will experience prostate enlargement, and nearly half will deal with erectile dysfunction after 40.
Ignoring symptoms doesn’t make them go away. Early screening, proper assessment, and evidence‑based care preserve urinary control, sexual confidence, and long‑term quality of life.
If you’re over 40, the earlier you start paying attention to your prostate, the longer you preserve your comfort, function, and independence.
Disclaimer: This article is for educational purposes only. Always consult a qualified healthcare provider regarding any prostate, urinary, or sexual health concerns.




